Specialized CARE

One of the many great things about being and RT is that the profession is dedicated to patients of all ages and circumstances. Maybe you’re interested in working with newborns or children. Or maybe you’re interested in the fast-pace world of transport. Wherever you want to take your career, respiratory care is there.
Here’s where you can take your respiratory therapy career:
LONG-TERM CARE
 Long-term care RTs work in skilled nursing facilities, subacute care centers, rehab hospitals, and other types of long-term care facilities. RTs in this area work with post acute and chronic disease patients who range in age from the very old to the very young.
Long-term care RTs work in skilled nursing facilities, subacute care centers, rehab hospitals, and other types of long-term care facilities. RTs in this area work with post acute and chronic disease patients who range in age from the very old to the very young.
What it takes: Most long-term care RTs enter the area after having worked in a hospital first, and most facilities will require therapists to hold the Certified Respiratory Therapist (CRT) credential. Many will also expect therapists to have the advanced level Registered Respiratory Therapist (RRT) credential as well, and therapists with the RRT are more likely to advance to managerial positions.
Neonatal-Pediatrics
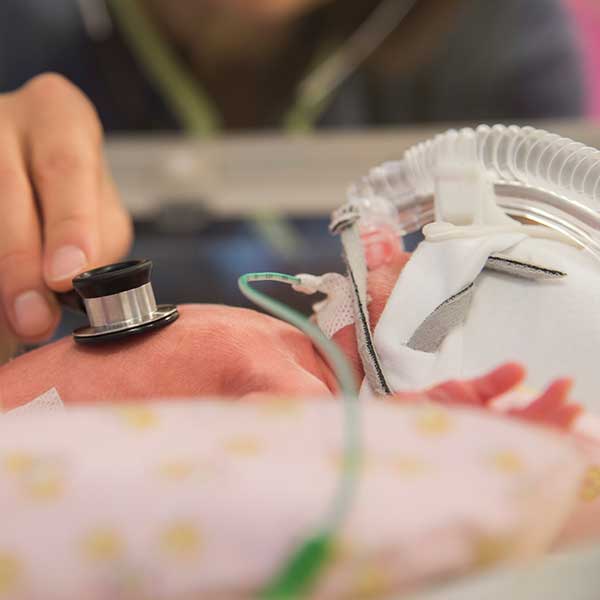
Neonatal-pediatric RTs work in children’s hospitals and general hospitals with neonatal-pediatric wards. Neonatal respiratory care involves treating and monitoring newborns for breathing disorders. A neonatal RT might monitor the breathing of premature babies, treat infants born with pulmonary diseases or disorders, or respond to the unique respiratory care needs of an infant in an emergency.
Pediatric RTs work with toddlers and older children, providing breathing treatments and other care for children with asthma, cystic fibrosis, and a wide range of other respiratory problems.
What it takes: Neonatal-pediatric therapists generally hold the CRT and/or RRT credentials, and many have also earned the Neonatal-Pediatric Specialist credential, or NPS. Increasingly, therapists who work with children with asthma are also earning the Asthma Educator-Certified credential, or AE-C, which certifies they are competent to counsel patients in asthma management.
Surface & Air Transport Transport

Surface and Air Transport RTs are a vital part of transport teams that treat critically ill patients in emergency transit to critical care units. These RTs do their job huddled in the back of a helicopter, air ambulance, or ground ambulance, working closely with nurses, physicians, and EMTs to keep patients alive and well until they can reach a hospital where they can receive necessary care. When they aren’t actively participating in a transport, these therapists work in other areas of their hospitals, from the emergency room to the intensive care units.
What it takes: Transport RTs earn the CRT and/or RRT credentials, and since many specialize in newborn and pediatric transports, the NPS credential as well. In addition, they may also be required to have one or more life support credentials.
Pulmonary Rehab

Pulmonary rehabilitation therapists help patients with chronic lung diseases like asthma, emphysema, chronic bronchitis, and pulmonary fibrosis cope with their conditions through education, treatment, and exercise. Most work in pulmonary rehabilitation centers, where they provide care and education to patients enrolled in their programs on an outpatient basis. But some also provide similar services to patients who are still in the hospital. Their primary goal is to help patients with chronic lung ailments breathe more easily and comfortably.
What it takes: Pulmonary rehab therapists will hold the CRT and/or RRT credentials. Many are also earning the AE-C, if asthma education is a part of their job responsibilities.
Polysomnography
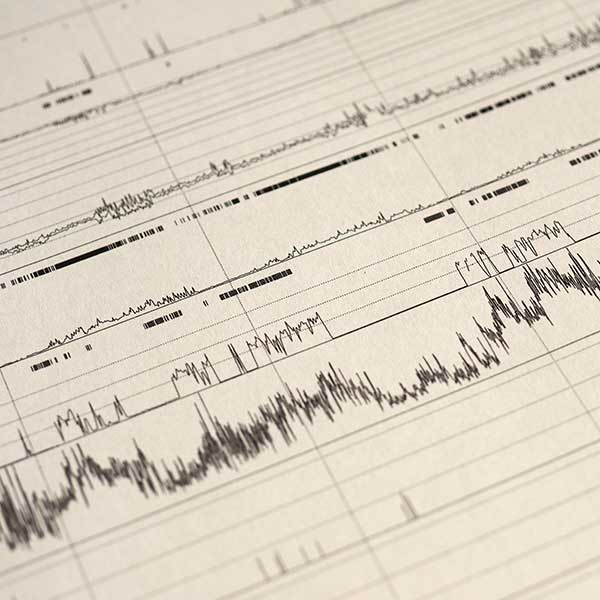
Over the past 30 years, sleep medicine technology has grown into a complex health care field, and respiratory therapists are increasingly being called upon to specialize in this dynamic area of care. RTs who work in sleep are generally employed by sleep laboratories, and they often work the night shift, when sleep studies are conducted.
General respiratory therapists can transition well into polysomnography, but most will need additional education and training to understand the 77 identified sleep disorders, to learn the function and use of polysomnographic equipment, and to provide safe and effective treatment to patients.
What it takes: RTs who go into sleep hold the CRT and/or RRT credentials, but may also want to earn the Registered Polysomnographic Technologist, or RPSGT, credential, which is awarded to those who take a specialty exam in polysomnography.
Education
Respiratory therapy education involves not just educating future practitioners, but also serving as an educational resource to practicing therapists. Respiratory therapy educators serve as professors and instructors in school programs, including those at the community college and university levels, and they may also work as continuing education coordinators for hospital RT departments.
What it takes: Most RT educators enter the specialty after having worked as a respiratory therapist in a hospital or other setting, and nearly all will have earned the advanced level RRT credential. Many educators also hold advanced degrees in education; in many schools, advanced degrees are considered essential for advancement.
Critical Care
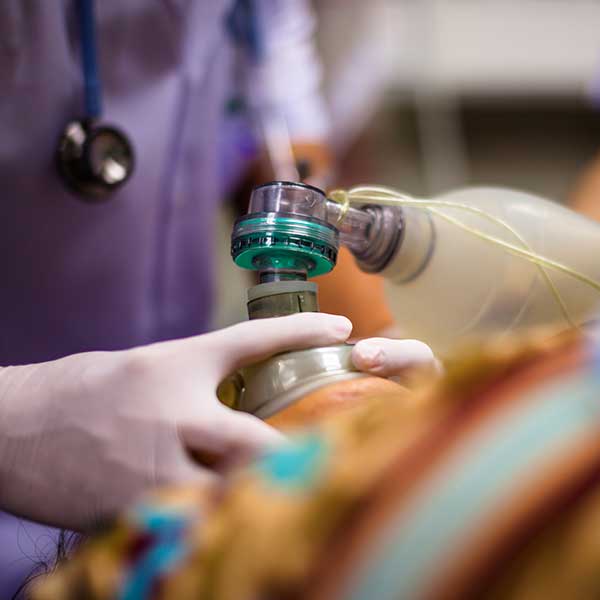
Many RTs love the fast pace and complex care delivered in the intensive care unit. Critical care respiratory therapists work with the most sophisticated equipment and the most severely ill patients.
What it takes: Therapists who staff the ICU most often have earned the advanced level RRT credential.
Case Management

Some RTs find it rewarding to develop a plan of care aimed at helping a patient transition from the hospital to the home care setting. These RT case managers help coordinate all aspects of a patient’s health care needs, making sure they have the equipment and other services they’ll need to recuperate at home.
What it takes: Most of these therapists hold the RRT credential, and many will also earn case management credentials as well, such as the Certified Case Manager, or CCM, credential.
Home Care

Many respiratory patients who have long-term illnesses like emphysema receive health care services in their homes from respiratory therapists. These therapists may work for a hospital, but most work for companies that provide home care equipment to people at home. RTs who like to visit with patients and be out and about do well in home care.
What it takes: Since home care requires a lot of independent thinking, most home care therapists have experience working in a hospital or other health care setting. Therapists will have earned the CRT and/or RRT credential, although the advanced level RRT credential is preferred by many home care companies.
Pulmonary Diagnostics

Therapists who enjoy the diagnostic aspects of respiratory care may specialize in pulmonary function testing. These therapists work in hospital-based or physician office-based pulmonary function laboratories, where they conduct the testing required to help physicians determine whether a person has a lung disease and, if so, which one.
What it takes: Therapists in this area generally earn the CRT and/or RRT credentials, but most will also earn specialty credentials in pulmonary diagnostics. These include the Certified Pulmonary Function Technologist, or CPFT, and Registered Pulmonary Function Technologist, or RPFT, credentials.
Management

Every respiratory care department has managerial personnel, and many RTs rise up the ranks to fill these positions. Managers in respiratory care are responsible for a wide range of duties — everything from staffing and budget preparation to setting policies and implementing directives from hospital administration.
What it takes: Managers typically enter the area after many years of experience as a staff therapist. Most will have earned the advanced level RRT credential, and many also earn bachelor’s degrees or above in business administration or public health.